This piece is the second in the Good News series on recovery and the good news that comes when people cut back or stop drinking alcohol or using drugs.
Jalie Tucker and her colleagues have recently published a significant review of the field of natural recovery from misusing drugs and alcohol (Tucker, Chandler, & Witkiewitz, 2020). It begins with a description of the scope of the problem.
“Substance use disorder (SUD) is among the most prevalent mental health disorders in the United States and in general clinical practice, with 7% of the U.S. population age 12 and older (19.7 million people) having an SUD of some kind in 2018. Alcohol use disorder (AUD) is the most prevalent SUD, with 5% of persons age 12 and older reporting AUD in 2018.”
These numbers do not include people whose drinking is heavy and risky, but does not meet the clinical criteria for an AUD diagnosis.
This graph developed by the Institute of Medicine is based on epidemiological data and population surveys. It illustrates the idea that the majority of people with alcohol problems are not at the severe end of the spectrum. Yet, people at the severe end are often the primary focus of policy, research, and treatment.
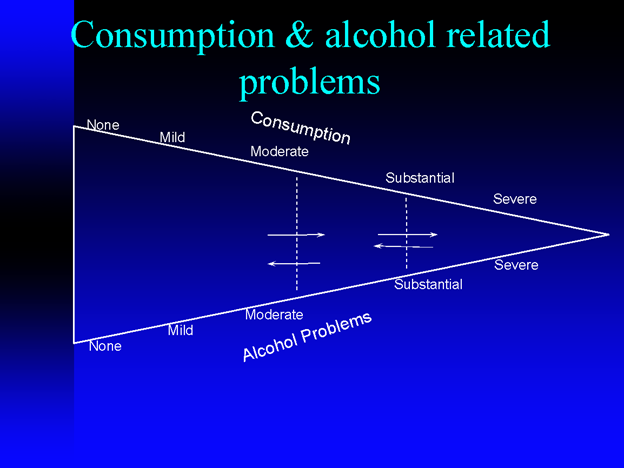
Note the arrows in the graph. They are meant to show that “both from an individual and a population perspective, consumption levels and the degree of problems vary from time to time.”
On average, heavy drinkers recognize that they have a drinking problem 10 years before they resolve their problem on their own or by seeking help (if they change at all) (Tucker & Simpson, 2011). While heavy drinking usually develops in young adults, natural recovery (and treatment seeking) tends to happen in mid-life. This data suggests that people are not in “denial” and recognize they have drinking problems long before they start to make changes or seek help. It indicates that other factors motivate and sustain change in drinking habits or drug use.
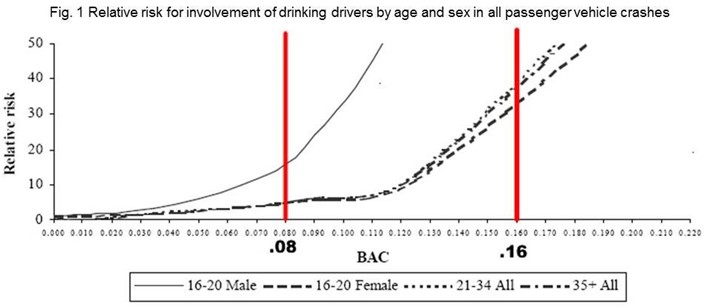
There is a dark side of natural recovery. Ten years is a significant chunk of a person’s life in which negative things are happening that are related to the person’s drinking or drug use. During this time, the person is at greater risk for severe problems. With alcohol we know that the higher a person’s blood alcohol concentration (BAC) is, the greater the risk for more serious problems that can be life threatening. Drinking and driving is one example. One’s risk for an alcohol-related crash increases exponentially as one’s BAC increases (see figure below). The red line at BAC of .08 is the limit for driving while intoxicated (DWI) in all states in the U.S. and the .16 line is the BAC limit for “aggravated DWI” in many states.
Now the good news. While few people will ever get treatment for their heavy drinking or substance use, about 70% will recover without professional help. This is not to say that they will cut back or stop drinking all on their own. We do know that having supportive family and friends increases the chances of a person resolving their drinking or drug misuse.
Speaking of family and friends, allow a brief aside. Our colleagues, Drs. Robert J. Meyers and Jane Smith have developed a program for friends and family members, and its effectiveness is supported by randomized clinical trials. They’ve published a self-help manual that provides guidance. It’s both appropriate for learning how to motivate a drinker or drug user to get treatment as well as how to support him or her when they are changing their drinking pattern. Highly recommended.
Fortunately for those thinking of changing their drinking or drug use, there are now evidence-based, self-guided programs that help people make these changes on their own. Our research team here at CheckUp and Choices have been developing, rigorously evaluating, and then making such programs available for over 25 years now. Our Drinker’s Checkup can help people increase their own internal motivation for change. For many, that’s all they need to make changes. We have also developed programs for people who want to cut back on their drinking or to stop drinking entirely. And we have programs for people who want to make changes to their drug use.
Our programs are based on cognitive behavioral and motivational enhancement interventions.
We recognize that whether or not you use online apps to make changes, having the support of others in your efforts is helpful. Family, friends, your local minister, and online mutual support groups like SMART Recovery and Moderation Management can provide the emotional support that many people find beneficial.

Dynamic Pathways to Recover from Alcohol Use Disorder is a newly published book by Drs. Jalie Tucker and Katie Witkiwietz (Eds.). It is a deep dive into the aspects of recovery and we highly recommend it for professionals as well as non-professionals who are interested in a comprehensive discourse on recovery. Chapter contributors include some of the most knowledgeable clinical researchers in our field.
This from the summary of the book on Amazon: Recovery from the disorder is a dynamic process of change, and individuals take many different routes to resolve their alcohol problems and seek to achieve a life worth living. Total abstention is not the only solution and robust recovery involves more than changing drinking practices. This volume brings together multidisciplinary research on recovery processes, contexts, and outcomes as well as new ideas about the multiple pathways involved. Experts chart the individual, social, contextual, community, economic, regulatory, policy, and structural influences that are vital to understanding alcohol use disorder and recovery. The book recommends new approaches to conceptualizing and assessing recovery alongside new avenues for research, community engagement, and policy that constitute a major shift in the practice and policy landscape.